Joint problems often occur locally when a person has pain in a particular joint and is able to pinpoint the exact location of the pain. However, sometimes joint pain cannot be localized because it affects all joints or several at the same time. In this case, it is too early to talk about rheumatoid arthritis, because in addition to this pathology, there are other diseases that affect all joints of the musculoskeletal system.
A careful doctor who will analyze the patient's complaints and determine the cause-and-effect relationship can determine the causes of pain in all joints at the same time. It is not always easy to diagnose, and it is not possible to distinguish a specific pathology immediately after a series of examinations with the most common symptoms. Therefore, if you experience systemic joint pain, do not delay seeing a doctor.
If all joints of the musculoskeletal system are seriously ill, the following reasons may occur:
- Pathologies of autoimmune origin and systemic allergic reactions.
- Rheumatoid arthritis.
- Osteoarthritis.
- Chronic fatigue, increased physical activity.
- Intoxication of the body.
- Blood diseases.
When pain occurs in several or all joints, it is important to remember that such a condition is only a reaction to certain diseases, but not independent diseases. The only exceptions may be pathologies such as osteoarthritis and rheumatoid arthritis when the cartilage itself is the immediate cause.
Rheumatoid Arthritis
The disease refers to chronic autoimmune pathologies in which the joints in the body are primarily affected. A distinctive feature of rheumatoid arthritis is the involvement of many joints in the pathological process.
At the same time, cytokines, metalloproteinase and chemotactic cytokines play a key role in the inflammatory process. These are anti-inflammatory elements that activate the human body's own immune cells. As a result, they spread to the site of inflammation, ie the joints of the human body, and cause a typical inflammatory reaction.A typical manifestation of rheumatoid arthritis is damage to the peripheral joints and symmetry. As the disease progresses, the pathology affects the larger joints. The pathology mainly affects women, it is three times less in men. It is diagnosed between the ages of thirty and fifty, but can sometimes appear in adolescents - the disease is called arthritis until adulthood.
Although scientists have clarified the immune features of the disease, it has not yet been possible to determine the exact cause of rheumatoid arthritis - why do anti-inflammatory cells acquire such pathological activity? To date, there has been evidence of a genetic predisposition to rheumatoid arthritis, and smoking, transmission of viral diseases, and other adverse factors have been shown to influence the appearance of pathologies.The course of the disease is caused by the activation of immune complexes produced by the synovial membrane and in the blood vessels. A rapid response to them are rheumatoid factors - antibodies produced by these complexes. In some cases, they appear on their own without the presence of provocative factors.
HELP!In the early stages of pathology, macrophages migrate to the affected areas, after which the number of lymphocytes increases. It causes the release of inflammatory mediators and the development of pathological processes throughout the body.
If there is a chronic damage to the synovium, instead of the usual thickness, it becomes denser and coarser, grows and wrinkles form on the surface. Cells in the synovial fluid produce stromelysis and collagenase, which contribute to destructive processes in cartilage tissue. The inflammatory process increases with the production of prostaglandins, fibrin deposits and necrotic processes occur.
Increased synovial tissue causes inflammatory mediators that help destroy not only cartilage but also bone tissue, ligaments and the joint capsule. The number of leukocytes in the joint fluid itself increases.
When the small joints of the body change shape and look ugly, they are covered with characteristic rheumatoid nodules. Such rheumatoid nodules contain necrotic parts of macrophages, fibroblasts and plasma cells. Similar nodules can be found in the internal organs.
The disease develops gradually. Patients suffer from general and local articular manifestations - in the morning there is a characteristic stiffness in the joints, fatigue is observed, there is anorexia, body temperature is subfebrile. The condition of the joints improves significantly an hour after waking up. The joints are affected symmetrically, and rheumatoid arthritis generally affects the following joints:
- Wrist.
- Second and third metacarpophalangeal.
- Shoulder.
- Knees.
- Ankles.
- Hip.
- Elbows.
In fact, the disease threatens any joint of the musculoskeletal system. Distal phalangeal joints and at the same time axial skeletal elements are least involved.
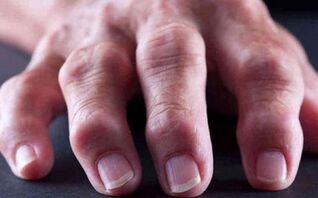
Joints ache, swell and redden, and become hot to the touch. To minimize painful sensations, patients try to bend their joints - this way there is less pain. The development of the disease occurs in the first 5-6 years after the appearance of the first pathological changes. Ten years after the development of the pathology, irreversible changes occur in patients.
During this period, patients develop significant joint deformities and instability may occur. Patients suffer from carpal tunnel syndrome when the nerve branches are compressed, and patients with rheumatoid arthritis of the knee joint may develop Baker's cyst, deep vein thrombosis, and so on.
In parallel with articular changes, every third patient has extra-articular manifestations of the body that develop with the development of pathology. Examples of such manifestations are rheumatoid nodules in the lungs, vasculitis, Felty's syndrome, myocarditis.
It is not difficult to diagnose the disease. Typical clinical criteria for rheumatoid arthritis are blood, erythrocyte sedimentation rate, significant C-reactive protein, and rheumatoid factor.
The health status of patients is shown in the form of an X-ray if rheumatoid arthritis is suspected. The disease differs from osteoarthritis, sarcoidosis, psoriatic arthritis and ankylosing spondylitis, arthritis developed on the background of hepatitis C.
Important!When diagnosing, it should be borne in mind that the disease has a very high mortality rate, but in rheumatoid arthritis it is not associated with joint damage, but with pathological changes in the heart, internal bleeding.
Treatment of the disease is carried out with supportive therapy in addition to strong NSAIDs. It is recommended to add exercise therapy, just to give a sufficient load to the joints. If necessary, surgery is performed.
Osteoarthritis
Osteoarthritis is another common pathology that can affect both large and small joints. Various factors can cause osteoarthritis, primarily affecting the cartilage tissue of the joint. In the human body, cartilage tissue performs several functions and is primarily a shock absorber during various movements. Constant stress causes increased wear on the cartilage.
If people with good health and strong immunity have a chance to repair damaged tissue, in older patients, as well as in patients with increased stress on the joint, the synthesis of new fibers is almost non-existent and cartilage tissue is not restored. Osteoarthritis is traditionally thought to be the result of a mechanical impact on tissues, but doctors now consider previously transmitted inflammatory diseases to be factors in the development of systemic osteoarthritis.
A typical symptom of the disease is pain in all joints, because the matrix loses extremely important substances - glucosamine and chondroitin sulfate. Deficiency of these elements leads to the emergence of the so-called joint, ie cracks form at different depths in the cartilage tissue.
Inflammatory processes can also disrupt the normal structure of cartilage tissue, so when it is localized in the subchondral part of the bone, doctors often diagnose microfractures in patients. The edges of the bone in the joint are covered with growths - osteophytes. They serve to compensate for the worn-out part of the cartilage, but in fact bring more negative feelings to patients.

Menopausal women are most susceptible to osteoarthritis.
Since the true cause of osteoarthritis has not been determined, doctors have identified several factors that contribute to the development of the disease:
- Congenital deficiency of cartilage tissue, which is very easy to damage. For example, patients with such a pathology develop flat feet, dislocations are often diagnosed - complete and incomplete.
- Sex is also one of the factors in the development of the disease, because according to statistics, osteoarthritis is twice as common in women as in men.
- Age feature - the disease generally develops in patients over the age of forty-five, occurs in women during menopause.
- Obesity.
- Metabolic problems.
- Increased sports load on the joints.
- Traumatic joint injuries.
The disease develops in any joint, but generally the starting joint has the greatest physical activity. In the knee joints, hips, elbows, etc. can be localized in.
The symptomatology of the disease is very clear, so osteoarthritis can not be missed. With an increasing load in a person, the joints immediately begin to ache, the intensity of the discomfort can vary: from a slight tingling in the joint to the most severe pain in the joint. Pain increases during exercise and is less pronounced at rest.
In parallel with the pain, patients suffer from the appearance of cracks and stiffness in the joints. Patients have limited mobility. Especially when the disease develops when reflex muscle spasms are added to the pathology.
In the later stages of the disease, patients develop a characteristic joint block - a sharp pain when the joint suddenly stops moving due to severe pain in the joint. This is due to the fact that pieces of cartilage tissue enter the cavity and impede movement. If the disease is accompanied by inflammation, there is swelling of the synovium, which is easy to see.
The development of osteoarthritis is very individual. In some patients, X-rays show signs of pathology, but the sensation does not change the picture of the disease. At the same time, other patients experience severe pain, inflammation and limited mobility when the joint in the picture itself appears satisfactory according to the stage of development of the pathology.
Diagnosis of the disease is based on X-ray data and clinical signs of the disease. In parallel, you can do an ultrasound or magnetic resonance imaging if you need to assess the presence of complications.
Doctors try to treat the disease taking into account the maximum protection of joint mobility and the patient's ability to work according to the profession. Therefore, it is extremely important in therapy to stop the development of the disease, relieve joint pain and eliminate inflammation.
Currently, the possibilities of treating osteoarthritis are not endless, and it is difficult to recognize the treatment tactics as successful, because it is impossible to restore the joints. The disease progresses to a chronic stage and must be fought continuously.
TIP!However, such unfavorable prognoses do not condemn patients to disability - with successful therapy you can learn to live with osteoarthritis and even continue physical activity.
Doctors use the following fund groups for treatment:
- Non-steroidal anti-inflammatory drugs.
- Glucocorticosteroids.
- Chondroprotectors.
- It is a tool to activate blood circulation.
- Muscle relaxants.
Disease therapy primarily consists of drugs that restore cartilage tissue to the maximum extent and can regulate metabolic processes in the joint. Therefore, the main emphasis is on the use of chondroprotectors, which begin immediately after the elimination of inflammation. Treatment with chondroprotectors is long-lasting, and the best results are seen only when treatment is started on time.
Other diseases
Rheumatoid arthritis and osteoarthritis are the most common pathologies in which the joints ache and ache on all sides of the body. However, in addition to disease leaders, there are other conditions that cause pain in the joints.
Joint pain may be a manifestation of leukemia.
Painful joints can be a manifestation of blood diseases. Hematological pathologies today are the most difficult not only for the attending physicians, but also in therapy. It is often combined with oncological factors, and diseases have a completely different meaning for the patient. In general, the joints in the body are aggravated by leukemia - acute and chronic. At the same time, patients do not doubt what this means, because the results of blood tests do not show abnormalities.
Arthralgia is not isolated, it affects not only the joint elements, but also the bones and muscles. Therefore, doctors advise patients with long-term pain, not only with an orthopedic traumatologist or surgeon, but also with a hematologist, who may suspect a pathology and send the patient for further examination.
Drunkenness is another cause of joint pain. The truth is that if the joints react very sharply to the body's absorption of toxins, and the joints begin to ache and bend, the effects of occupational hazards, drunkenness with household waste, tobacco smoking, and alcoholism may be to blame. Patients suffer from extremely unpleasant symptoms - all joints ache, as if the flu affects the general condition of the body.
Improving patients' health is possible after diagnosis. Detoxification treatment is performed, the blood is cleansed, and as a result, the joint fluid is removed from the toxins.
Most Important
Pain in all joints of the body is not always associated with the pathology of the joints themselves. If the joints of the body are affected, the common cause is rheumatoid arthritis or osteoarthritis. Symptoms increase rapidly and the pathological process in the joints progresses.
In other cases, when joint pain is not associated with joint damage, anxiety may be a manifestation of systemic diseases, such as blood leukemia, as well as osteoporosis, intoxication of the body, infection. It is not easy to cope with the disease, but it is more difficult to diagnose the disease. Patients with the appearance of pain in the joints should go to the clinic in time to start treatment at an early stage.
























