
Osteochondrosis is one of the most common pathologies of the spine. It is believed to develop mainly in the neck or lumbar region. After all, it is in these places that the spine is very mobile and under great stress. However, for most people, a sedentary lifestyle and sitting at a table for long periods of time have made osteochondrosis of the thoracic spine more and more common. Although in many cases this pathology is not diagnosed immediately. After all, the peculiarity of thoracic osteochondrosis is that its symptoms are nonspecific and similar to many other pathologies.
common features
This degenerative-dystrophic disease affects the intervertebral discs of the thoracic spine. This is due to the disruption of metabolic processes that cause thinning and drying of cartilage tissue. As a result, under the influence of physical load, the discs begin to collapse and lose their cushioning function. The vertebrae, ligaments and joints in the spine are gradually affected. Nerve fibers and blood vessels can be damaged.
This process develops slowly, so the diagnosis of pathology is difficult. In addition, not everyone sees a doctor right away because they do not know the dangers of thoracic osteochondrosis. But without treatment, the disease can cause serious complications. Because this part of the spine is responsible for the blood supply and innervation of the internal organs, various pathologies can develop with an advanced form of thoracic lumbar osteochondrosis. Intestinal peristalsis, heart, liver and digestive system are disturbed. Pancreatitis, cholecystitis, biliary dyskinesia may appear. But most complications appear in the spine. In addition to intervertebral disc herniation and intercostal neuralgia, spinal cord compression, spondylosis, sciatica, and posture disorders may develop.
Osteochondrosis of the thoracic spine is equally common in men and women. Appearance does not even depend on age, although previously it was believed that degenerative-dystrophic diseases are characteristic only of the elderly. However, modern youths are increasingly suffering from osteochondrosis due to improper diet and sedentary lifestyle.
The most common osteochondrosis is believed to be cervical. It often occurs in the pathological lumbar region. This is due to the special structure of the skeleton. In the thoracic region, the spine is less mobile because it joins the ribs and sternum.
Here, the intervertebral discs are thinner and the vertebrae are closer together. However, this part is less susceptible to injuries and other external influences, because part of the load is taken by the ribs and chest.
Osteochondrosis usually appears at the level of 7-11 vertebrae. In this case, primarily the intervertebral discs are affected. Often 1-2 segments of the spine are affected. However, sometimes polysegmental osteochondrosis develops, in which several discs are destroyed at the same time. Rarely, pathology in this section occurs independently, usually associated with cervical or lumbar spine injury. In this case, the symptoms are more pronounced, so the disease is easier to diagnose.
The peculiarity of thoracic osteochondrosis is that it rarely manifests itself with back pain after tension, as it is localized in the cervical or lumbar region. The pathology is initially confused with heart or lung disease. After all, the pain is often localized in the chest, shortness of breath, nausea, tremors appear. However, the manifestations of thoracic osteochondrosis are not very bright, so patients do not always go to the doctor at an early stage. Therefore, the pathology progresses.
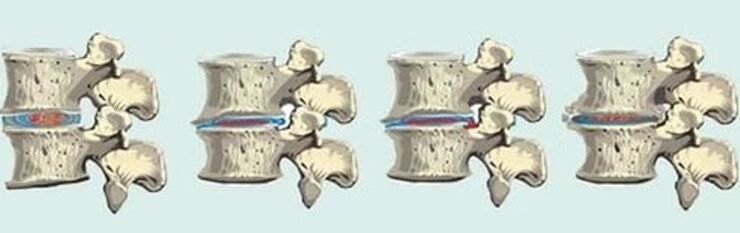
Development of the disease
The danger of thoracic osteochondrosis is that it is "masked" like other diseases. The pathology develops slowly, rarely any of the patients consult a doctor at an early stage. Osteochondrosis begins with thinning of the intervertebral disc. Its nucleus flattens, the cortex cracks and dries, and the vertebrae come together. There is usually no serious discomfort at this stage, only mild muscle tension. If the disease is detected, then it can be completely cured by restoring the condition of the discs.
However, in general, the development of osteochondrosis continues. An inflammatory process may begin in the surrounding soft tissues, the joint capsules suffer. Decreased mobility of the spine, vertebral displacement may occur. If increased physical activity continues, micro-cracks appear in the vertebrae due to friction. In this case, there is a feeling of tightness in the chest, pain in the upper part of the body with any movement.
In the third stage of osteochondrosis, the intervertebral discs become very thin, protrusions and hernias appear. The mobility of the spine is almost completely limited. Osteophytes begin to form in the spine. This stage is characterized by an open radical syndrome due to damage to nerve fibers. In this case, the work of internal organs is seriously impaired. In most cases, this is when the patient sees a doctor and begins treatment. If this is not done, complications can lead to disability, and when the spinal cord is compressed, it can lead to complete immobility.
The final stage of osteochondrosis is characterized by complete destruction of the discs and loss of their function. The bone tissue of the spine begins to collapse, so the mobility of the spine is completely impaired. All vegetative and radical symptoms of thoracic osteochondrosis are clearly expressed.

The development of thoracic osteochondrosis is wavy. This is a chronic process that usually goes on slowly, with little anxiety. There may be increased fatigue, weakness. And when exposed to external factors, an exacerbation occurs with sharp pains. In this condition, patients are often hospitalized because the attack may be accompanied by a feeling of shortness of breath, difficulty breathing, chest or abdominal pain.
Reasons
The main cause of thoracic osteochondrosis, as in other forms, is a violation of mineral metabolism. As a result of degenerative-dystrophic processes, protrusion or disc herniation occurs, they become thinner and cease to perform their functions, the vertebrae gradually collapse, and osteophytes grow. This is most often due to a lack of essential nutrients or an unbalanced diet that causes age-related changes in the composition of cartilage tissue. Disc degeneration can also lead to deterioration of blood circulation in the spine, bad habits or hereditary predisposition.
However, lack of minerals does not always lead to osteochondrosis. This requires stimuli that affect the spine itself.
Therefore, the following causes of this pathology are also distinguished:
- frequent static loads on the spine;
- sitting at a table for a long time in an uncomfortable position;
- lift weights;
- obesity;
- damage to the spine or surrounding tissues;
- to engage in power sports;
- raxiokampis;
- weakness of the muscle corset;
- congenital defects of the skeleton;
- severe hypothermia;
- nervous tension.

It has been found that people who have been restless at the table or driving for a long time, as well as those who do heavy physical work, are most susceptible to the development of pathology. Indeed, both increasing loads and their complete absence are equally detrimental to intervertebral discs.
In addition, osteochondrosis often develops in young people with osteochondropathy. This pathology usually develops in the lower thoracic region in adolescents. It is characterized by necrosis of the sponge tissue of the vertebrae, deformity of the spine and the appearance of neurological symptoms. Complicated by osteochondrosis with the development of pathology.
Manifestations of pathology
The main symptoms of osteochondrosis of the thoracic spine are pain, radicular syndrome and dysfunction of internal organs. In this pathology, the pain may be acute, paroxysmal or painful, constant, increasing with movement. Sometimes patients are hospitalized on suspicion of acute pancreatitis, cholecystitis or urolithiasis. After all, pain is not always localized in the affected vertebrae. Therefore, thoracic osteochondrosis is often confused with pathologies of other organs.
In addition, degenerative processes in the spine in this disease are almost always accompanied by vascular disorders or intercostal neuralgia. This is due to the special structure of the spine in this section - a small distance between the vertebrae and many nerves and blood vessels.
Thoracic osteochondrosis can be suspected by restricting the mobility of the upper body and increasing flexion. Intercostal neuralgia is common. Acute pain can last for several hours or more. Lifting weights, maintaining a static posture for a long time, can be triggered by hypothermia.
If the vessels are affected, there is a violation of the blood supply and nutrition of the skin. For this reason, the fragility of the nails, dryness and swelling of the skin increases. Coldness of the skin and coldness of the limbs are often observed.
Features of pain
In osteochondrosis of the thoracic region, the pain may vary in intensity and localization. The pain usually occurs between the chest or shoulder blades. They are aggravated by raising the arm, turning or bending the body, coughing or sneezing. The pain can be sharp, squeezing, painful.
Such feelings are usually divided into two groups: dorsal and dorsal. Dorsago is an attack of sharp pain between the shoulder blades. It is also called "chest lumbago". The pain is so severe that it prevents a person from moving. Dorsal attack usually occurs after a long stay in a stationary position in the first movement. It is accompanied by muscle spasms, so respiratory function is impaired. The sensation extends to the backbone, from the ribs to the chest. Chest pain with osteochondrosis is similar to an attack of angina pectoris, but unlike it, it is not removed by nitroglycerin. In addition, the pain increases when pressing on the vertebrae.
Dorsalgia is a chronic, mild pain. It usually begins gradually with a slight feeling of discomfort in the thoracic spine. In this case, the pain may be exacerbated when bending, turning, raising the arm, and even walking. This severely limits the patient's mobility. In addition, an increase in pain may be observed with deep breathing, after a long stay in a sitting position, or at night. Dorsalgia can last from 2 weeks to a month. Chest tightness and shortness of breath are similar to pneumonia, but the patient does not have a cough or fever.
Radicular syndrome
When the vertebrae or spasmodic muscles of the nerve roots are compressed, the symptoms of osteochondrosis of the thoracic region become more pronounced. After all, the spinal nerves located in this part of the spine are responsible for the innervation of the skin, the motor functions of the extremities and the activity of internal organs.
In addition to pain in the back, chest or abdomen, nerve compression is accompanied by the following symptoms:
- paresis or partial paralysis of the limbs;
- violation of skin sensitivity;
- numbness, burning, tingling, a feeling of running "goose shoots";
- violation of tendon reflexes;
- reflex muscle spasm;
- Trophic changes in the skin - hair loss, discoloration, dryness and peeling.
The intensity of these symptoms increases after physical exertion, deep inhalation, prolonged sitting, hypothermia or stress.
Vegetative disorders
The thoracic spine has many nerves and blood vessels that support the normal functioning of the internal organs. Therefore, various autonomic disorders with osteochondrosis are inevitable. They depend on the localization of the affected vertebra, as well as the stage of pathology.
With lesions of the spine in the upper thoracic region, there is discomfort in the esophagus, a feeling of coma in the pharynx. Difficulty swallowing, sound changes may appear. The middle thoracic vertebrae are responsible for the liver, gallbladder, stomach and pancreas. Therefore, when they are destroyed, the symptoms often appear as pancreatitis, cholecystitis or gastritis. If the degenerative changes have affected the lower thoracic vertebrae, there may be problems with the intestines and genitals.
Patients often consult a doctor with abdominal pain. They usually worsen in the evening or after physical activity. Moreover, the pain is not related to the characteristics of the patient's diet. This gastrointestinal syndrome is characteristic of thoracic osteochondrosis. However, despite abdominal pain, intestinal upset, nausea and bloating, there are no problems with the digestive system. These feelings are caused by damage to the nerves and blood vessels in the spine.
Diagnostics
Due to the nonspecific symptoms of thoracic osteochondrosis, the pathology can be detected only by a thorough examination. At the same time, it is very important to distinguish it from other diseases. X-ray or tomography of the spine helps to rule out spondylopathy, rheumatoid arthritis, ankylosing spondylitis.
However, other examination methods are also needed. This includes a urine test, a general and biochemical blood test, fluorography, ECG, MRI or ultrasound of the internal organs. Such an examination allows to exclude pathologies such as pancreatitis, gastritis, gastric ulcer, heart attack, pneumonia and urolithiasis.

Treatment
Treatment of osteochondrosis of the thoracic spine should be comprehensive. Since the cause of the pathology is degenerative processes, it is impossible to completely cure it. Only in the initial stage, when the structure of the vertebrae is still intact and slightly reduced in the size of the discs, it is possible to stop this process and restore the function of the spine.
However, in general, treatment of thoracic osteochondrosis aims to slow tissue destruction, relieve pain and neurological symptoms, and restore mobility. The choice of therapeutic methods depends on the stage of the pathology, the location of degenerative processes, the symptoms. Treatment should be started as early as possible, then there is more chance to avoid complications.
It is especially important to consult a doctor if you have severe back pain and shooting pain spreads to the chest or shoulder blade. Such a complication can be eliminated by special methods. These are usually drugs used in the form of tablets or injections, various ointments or compresses, physiotherapy procedures. Spinal immobilization is also required: the patient is shown bed rest and restricted movement for several days.
Treatment is not stopped after the seizure is removed. But now its main goal is to stop the degenerative processes and restore tissue trophism. To do this, drugs are used chordroprotectors, vitamins and means to improve metabolism. In addition, mandatory massage courses and physiotherapy procedures, as well as physiotherapy exercises are prescribed. In addition, special exercises should be performed regularly. To prevent complications, it is necessary to control the diet to provide the body with all the necessary vitamins and minerals. Lifestyle is also very important: choose the right mattress and pillows for sleeping, chairs for work, alternative rest and physical activity.
Osteochondrosis of the chest is a fairly serious pathology that can lead to dangerous complications if left untreated. However, difficulties in diagnosis often lead to the progression of the disease. Therefore, it is very important to lead a healthy lifestyle and avoid the factors that lead to the destruction of discs. This will help prevent the development of osteochondrosis and keep the spine healthy.

























