Coxarthrosis of the hip joint (HJ) is a degenerative-dystrophic disease that affects cartilage and bone tissue. In medical articles it can be called differently: deforming coxarthrosis, DOA of the hip joint, osteoarthritis. All these terms mean the same pathology - osteoarthritis, but "coxarthrosis" is a narrower concept that characterizes the defeat of the hip joint.
Osteoarthritis first affects the cartilage, then the bones and surrounding structures - ligaments and muscles - are involved in the pathological process. If there are changes in the bones, the prefix "osteo" is added to the word "osteoarthritis". In advanced cases, the joint is deformed and they talk about osteoarthritis, which is already deformed.
common features
Deformative osteoarthritis of the hip joint is the second most common after knee gonarthrosis. Due to the deep location of the hip joint, the bone deformity may remain unnoticed for a long time, and only in later stages will changes be seen in the X-ray images taken.
The development of this disease is influenced by various factors, including inactive lifestyle, trauma and metabolic disorders. Due to the nature of modern life, which is often not a place for physical education, osteoarthritis affects more and more people. In addition, the peak incident falls on the middle age group - from 40 to 60 years.
Reference:coxarthrosis often affects women more than men.
Development mechanism
The femur is made up of two bones: the femur and the iliac crest. The head of the femur enters the pelvis, which remains motionless during movement - walking, running. At the same time, the articular surface of the femur can move in several directions, providing flexion, extension, abduction, adduction, and rotation (rotation) of the thigh.
During physical activity, the femur moves freely in the acetabulum thanks to the cartilage tissue surrounding the joint surfaces. Hyaline cartilage is distinguished by its strength, firmness and elasticity; acts as a shock absorber and participates in the distribution of the load during human movements.
Inside the joint is the synovial fluid, the synovium, which is important for the lubrication and nourishment of cartilage. The whole joint is surrounded by a dense, thin capsule surrounded by strong muscles of the thigh and hip. These muscles also act as shock absorbers to prevent damage to the hip joint.
The development of coxarthrosis begins with a change in the viscous and thickening joint fluid. Due to the lack of moisture, the cartilage is not sufficiently nourished and begins to dry out, loses its smoothness and cracks appear on it.
The bones are no longer able to move as freely as before, and they rub against each other, causing micro-damage to the cartilage. The pressure between the bones increases, the cartilage layer becomes thinner. Under the influence of increasing pressure, the bones are gradually deformed, local metabolic processes are disrupted. In the later stages, there is acute atrophy of the leg muscles.
Reasons
Deformative arthrosis of the hip joint can be primary or secondary. It is not always possible to determine the cause of primary osteoarthritis. Secondary osteoarthritis appears against the background of existing diseases, namely:
- congenital femoral dislocation or femoral dysplasia;
- Perthes disease (aseptic necrosis of the femoral head);
- coxarthritis of the hip joint of infectious, rheumatic or other origin;
- pelvic bone damage - dislocations, fractures.
Dysplasia of the hip joint is a congenital defect, sometimes not manifested clinically for a long time, and can lead to the development of dysplastic coxarthrosis in the future (25-55 years).
Coxsackie's arthrosis can be left-sided, right-sided, and symmetrical. Primary osteoarthritis is often accompanied by diseases of the musculoskeletal system - especially osteochondrosis and gonarthrosis.
There are also risk factors that contribute to the onset of the disease:
- excessive weights and excessive loads on the joints;
- disorders of blood circulation and metabolism;
- hormonal changes;
- curvature of the spine, straight legs;
- old age;
- hypodynamics;
- heredity.
It should be noted that coxarthrosis itself is not hereditary. However, certain features of the metabolism or structure of connective tissue may create the preconditions for the development of osteoarthritis in a child in the future.
Symptoms of coxarthrosis
The leading symptom of osteoarthritis of the hip joint is pain in the hips and groin of varying intensity. There is also a change in gait due to stiffness and stiffness during movement, a decrease in muscle volume, shortening of the affected joint, and lameness.
Coxarthrosis progresses most slowly, causing discomfort first and mild pain after exertion. But over time, the pain increases and appears at rest.
A typical manifestation of the pathology is the difficulty in missing a hip when a person is unable to "jump" in a chair. The presence and severity of coxarthrosis symptoms depend on its severity, but pain syndrome is always present.
There are three degrees or types of osteoarthritis of the thigh, depending on the severity of the injury and the accompanying symptoms:
- 1 degree. The thigh hurts not all the time, but from time to time, especially after walking or standing for a long time. The pain syndrome is localized in the joint area, but can sometimes spread from the feet to the knees. Grade 1 coxarthrosis muscles do not decrease in size, gait does not change, motor ability is fully preserved;
- 2nd degree. The pain intensifies, not only after running or walking, but also at rest. The pain is more common in the thigh area, but can spread to the knee. It is painful to press on a damaged limb during heavy loads, so the patient begins to feel pain in his legs and limbs. The range of motion in the joint is reduced, making it particularly difficult to move the foot to the side or rotate the hip;
- 3 degrees. The pain is permanent and does not last even at night. The gait is markedly impaired, independent movement is significantly complicated, and the patient leans on a cane. The range of motion is sharply limited, atrophy of the muscles of the hip and the whole leg, including the lower leg.
- Due to muscle weakness, the pelvis bends forward, the affected leg shortens. To compensate for the difference in the length of the limbs, the patient bends his body to the affected side while walking. This causes a change in the center of gravity and increased stress on the affected joint.
Osteoarthritis or Osteoarthritis?
Arthritis is a joint inflammation that can be an independent disease or develop against the background of systemic pathologies (eg, rheumatism). In addition to the inflammatory response, symptoms of osteoarthritis (especially in the advanced stages) include limited mobility and changes in the shape of the joint.
Degenerative-dystrophic changes in osteoarthritis are based on the defeat of cartilage tissue, which often leads to the appearance of inflammation. Therefore, osteoarthritis is sometimes called osteoarthritis. Because osteoarthritis is almost always associated with joint deformity, the term "osteoarthritis" is applied to it.
Reference:According to the International Classification of Diseases (ICD-10), osteoarthritis and osteoarthritis are the same types of pathology.
Diagnosis of coxarthrosis
The diagnosis of "coxarthrosis of the hip joint" is made on the basis of examination, patient complaints and examination results. The most informative method is X-ray: in the pictures you can see both the degree of damage to the joint and the cause of the disease.
For example, in hip dysplasia, the acetabulum is more straight and inclined, and the cervico-diaphyseal angle (vertical curvature of the femoral neck) is larger than normal. Perthes' disease is characterized by deformity of the femur in the immediate vicinity of the joint.
Grade 3 coxarthrosis is characterized by narrowing of the joint space, enlargement of the femoral head, and numerous bone growths (osteophytes).
If the patient has a fracture or dislocation, X-rays will also show signs of trauma. If a detailed assessment of the condition of the bones and soft tissues is required, magnetic resonance imaging or computed tomography may be ordered.
Differential diagnosis is made with the following diseases:
- gonarthrosis;
- osteochondrosis and radicular syndrome;
- trochanteritis (inflammation of the trochanteric bone of the thigh);
- ankylosing spondylitis;
- reactive arthritis.
Decreased muscle volume with grade 2 and 3 coxarthrosis can cause pain in the knee area. In addition, the knee often hurts more than the hip joint itself. An X-ray is usually sufficient to confirm the diagnosis and rule out gonarthrosis.
With diseases of the spine - osteochondrosis and compressed nerve roots - the pain is very similar to coxarthrosis. However, it occurs unexpectedly after an unsuccessful movement, a sharp turn of the body or lifting weights. The pain begins in the gluteal region and spreads to the back of the foot.
Radicular syndrome is characterized by severe pain when lifting a straight limb from a stretched position. However, as in coxarthrosis, there is no difficulty in pushing the foot to the side. It should be noted that osteochondrosis and osteoarthritis of the hip joint are often diagnosed at the same time, so a thorough examination is required.
Trochanteritis, or trochanteric bursitis, develops rapidly, unlike osteoarthritis, which can develop slowly over years and even decades. The pain syndrome develops within a week or two, although it is very intense. The cause of trochanteritis is trauma or excessive exercise. Movement is not limited and the leg is not shortened.
Ankylosing spondylitis and reactive arthritis may also be accompanied by symptoms that mimic coxarthrosis. The symptom of such diseases is the appearance of pain mainly at night. The hips can hurt very badly, but the pain decreases when walking and moving. In the morning, patients are worried about the stiffness that disappears after a few hours.
Treatment of osteoarthritis of the hip joint
Coxarthrosis can be treated conservatively or surgically. The choice of treatment depends on the stage and nature of the pathological process. If grade 1 or 2 disease is detected, it is treated with medication and physiotherapy. Therapeutic exercises and massage are added to them after the elimination of acute symptoms. If necessary, a special diet is prescribed.
The sooner coxarthrosis is detected and treated, the better the prognosis. With the help of drugs and therapeutic measures, the pathological process can be significantly slowed down and the quality of life can be improved.
Non-steroidal anti-inflammatory drugs (NSAIDs) are used to relieve pain and inflammation. It should be noted that anesthesia is performed as soon as possible, because NSAIDs can adversely affect the digestive system and slow down the recovery process in cartilage tissue.
With the help of chondroprotectors it is possible to accelerate the recovery of cartilage. However, these drugs are effective only in the early stages of the disease, when its hyaline cartilage is not completely destroyed. Chondroprotectors are prescribed in the form of tablets or intraarticular injections.
Vasodilators are used to improve joint blood supply. Muscle relaxants are recommended for muscle spasms.
In the case of persistent pain syndrome, which is difficult to eliminate with pills, injections are made into the hip joint. Corticosteroids relieve inflammation and pain well.
Drug therapy can also be supplemented with local agents - ointments and gels. They have no obvious effect, but help to cope with muscle spasms and reduce pain.
Physiotherapy helps improve blood circulation and cartilage nutrition. Procedures such as shock wave therapy (SWT), magnetotherapy, infrared laser, ultrasound and hydrogen sulfide baths for coxarthrosis have proven to be excellent.
Operation
In stage 3, the treatment of osteoarthritis can only be surgical, because the joint is almost completely destroyed. Partial or total arthroplasty is performed to restore the function of the hip joint.
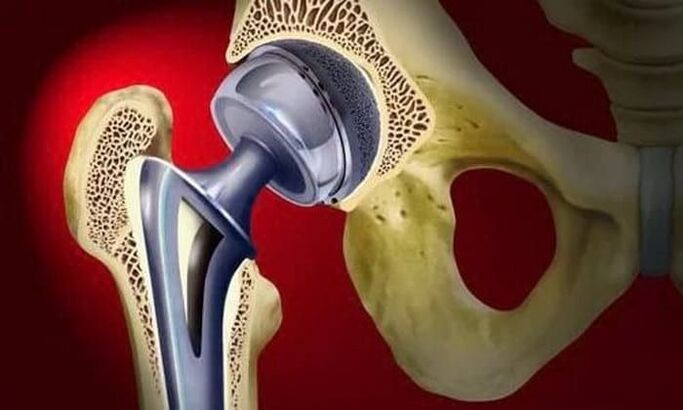
In cases of advanced osteoarthritis, surgical treatment is recommended when conservative therapy is weak.
In partial prostheses, only the head of the femur is replaced with an artificial prosthesis. Total prosthesis means replacement of both the femoral head and the acetabulum. The operation is performed under general anesthesia, and in most cases (approximately 95%) the function of the hip joint is completely restored.
During rehabilitation, the patient is prescribed antibiotics to prevent infectious complications. On days 10-12, the sutures are removed and exercise therapy begins. The attending physician helps the patient to learn to walk and to distribute the load properly to the operated limb. Exercise is an important step to increase muscle strength, endurance and flexibility.
Ability to recover is restored on average 2-3 months after surgery, but for older people this period can be up to six months. After rehabilitation, patients can fully move, work and even exercise. The service life of the prosthesis is at least 15 years. A second operation is performed to replace the worn prosthesis.
Effects
Without timely and adequate treatment, coxarthrosis can not only significantly worsen the quality of life, but can also lead to disability and disability. Already in the second stage of osteoarthritis, the patient is given the 3rd disability group.
When shortening the affected joint by 7 cm or more, a second group is assigned when a person moves only with the help of improvised means. Group 1 disability is accepted by patients with grade 3 coxarthrosis accompanied by complete loss of motor ability.
The recommendations for medical and social examination (CEC) are:
- long course of osteoarthritis, more than three years, with regular exacerbations. The frequency of exacerbations is at least three times every 12 months;
- underwent endoprosthetic surgery;
- severe disorders of the musculoskeletal system of the extremities.
Prophylaxis
The main measures to prevent coxarthrosis are diet (if you are overweight) and regular but moderate physical activity. It is very important to avoid damage to the pelvic region and hypothermia.
Swimming is beneficial in the presence of risk factors for the development of osteoarthritis, as well as in all patients with the diagnosed disease. Sports such as running, jumping, football and tennis are not recommended.

























